Current Projects
Learn more about our active projects here:
Year 13 (2025-2026) Projects
Principal Investigator: Brooke Lombardi, PhD, MSW

Limited geographic access to obstetric care jeopardizes timely, high-quality maternity care and contributes to preventable maternal morbidity and mortality, especially in rural and underserved areas of the United States. Strengthening the obstetric workforce through targeted training capacity is one potential strategy to address these access gaps. This study will examine the geographic distribution of hospitals with an obstetric unit and the location of obstetrics and gynecology (OBGYN) residency training sites using drive-time analysis. The study will utilize administrative and publicly available datasets to identify areas with obstetric services and will assess travel time between women of childbearing age and delivery hospitals. As obstetric unit closures continue to rise in both urban and rural hospitals across the United States, this project provides an update to maternity care access and highlights where training capacity could be expanded to help reduce disparities in maternal health outcomes.
Principal Investigator: Brianna Lombardi, PhD, MSW

Nutritionists and registered dietitians (RDs) are essential healthcare professionals who provide medical nutrition therapy, preventive nutrition services, and health promotion programs to address diet-related chronic diseases and improve population health outcomes. This study will compare five national data sources to understand the size and geographic distribution of the nutrition workforce in the United States, examining variations in workforce estimates by source, geography, and state regulation.
What proportion of rural areas are Health Professional Shortage Areas?
Principal Investigator: Erin Fraher, PhD, MPP
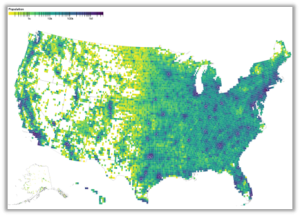
Some estimates suggest that 66.5% of primary care HPSAs are in rural areas; however, it is unclear what proportion of all rural areas are primary care Health Professional Shortage Areas (HPSAs). This project will assess the proportion of rural areas, using different measures of rurality, that are designated as HPSAs and characterize the population living in rural areas that are not designated HPSAs.
Developing A Better Understanding of How The HPSA Designation Process Varies between States
Principal Investigator: Erin Fraher, PhD, MPP
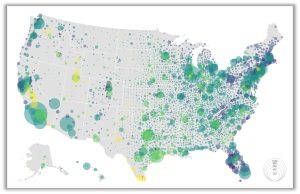
The Primary Care Health Professional Shortage Area (HPSA) designation process is a critical tool for identifying areas and populations with insufficient access to primary care clinicians. This study examines and documents the differences and similarities in data collection, analytical methods, and decision-making processes used by states to designate HPSAs.
Ongoing Projects
![]() Visualizing Trends in Foreign-Born and Foreign-Trained Physicians Working in the United States
Visualizing Trends in Foreign-Born and Foreign-Trained Physicians Working in the United States
Investigators: Brianna Lombardi, PhD, MSW, Evan Galloway, MPS, Brooke Lombardi, PhD, MSW, Erin Fraher, PhD, MPP
As the United States faces worsening workforce shortages and a persistent maldistribution of health care workers, foreign-born and foreign-trained health professionals may comprise an increasingly important labor source. We will develop a data visualization that allows users to explore the demographic, practice, and geographic characteristics of this workforce, as well as their origin-countries and their destinations in the United States.
![]()
Understanding States’ Use of Alternative Pathways for Foreign-Trained Physicians
Investigators: Erin Fraher, PhD, MPP Colleen Tapen, MPH, MBA, Haley Simons, Emily Hawes, PharmD, BCPS, CPP
An increasing number of US states are allowing international medical graduates (IMGs) to pursue alternative pathways to residency, licensure, and practice, in some cases bypassing the requirement to complete a US residency. In this study, we will interview experts from states pursuing alternative pathways for IMGs to understand the types of alternative pathways being developed, states’ motivations in pursuing these pathways, their design and implementation, and the degree to which they are measuring the outcomes of these changes.
![]()
Understanding Trends in Nurse Practitioner Turnover by Setting
Investigators: Esita Patel, PhD, Erin Fraher, PhD, MPP
It is unclear how the COVID-19 pandemic affected turnover of Nurse Practitioners (NP) and how NP turnover varies by setting. This study will compare NP workforce behaviors (e.g., turnover rates, intention to leave, and reasons for leaving or staying) during the pre-pandemic (2018) and mid-pandemic (2022) periods in hospital and outpatient settings.
![]()
Colocation of Primary Care, Dental, and Pharmacy Residencies: An Analysis of Interprofessional Post-Graduate Training
Principal Investigator: Emily M. Hawes, PharmD, BCPS, CPP
An integrated, interprofessional team-based model of practice is an essential element of delivering high- quality primary care. Integrating dentists and primary care physicians enhances access and coordination of care. Despite support for interprofessional education across national health organizations and accrediting bodies, little is known about the prevalence and composition of interprofessional post- graduate training on a national level. This project will produce a much-needed body of evidence on the prevalence, location and factors predicting co-location of dental, pharmacy and primary care residencies in the United States.
The aims of this study are:
- Identify the proportion of pharmacy and primary care physician post-graduate training programs that are collocated.
- Identify the proportion of pharmacy, dental, and primary care physician post-graduate training programs that are collocated.
- Examine predictors of pharmacy and primary care post-graduate training program colocation as well as pharmacy, dental, and primary care post-graduate training program colocation [such as program sponsor, residency specialty/size, training setting (e.g., FQHC, hospital.), state, and measures of underservice (e.g., Area Deprivation Indices, metro/non-metro)].
![]() Using Latent Transition Analysis as A Tool to Understand How Physician Careers Evolve over the Life Course
Using Latent Transition Analysis as A Tool to Understand How Physician Careers Evolve over the Life Course
Principal Investigator: Erin P. Fraher, PhD, MPP
In a Year 10 study, we used latent class analysis (LCA) to describe the career typologies of primary care physicians (PCPs) in North Carolina which found that PCPs were sorted into four types of careers in 2009 and 2019 with high class separation and classification certainty in both years (entropy = 0.98, mean posterior probabilities > 0.9). Key attributes that predicted career type were whether the PCP practiced in a rural vs urban area, hospital vs. ambulatory care settings, and whether they provided prenatal and obstetric care. We found statistically significant differences in PCPs’ characteristics (sex, age, race/ethnicity), medical school location (IMG vs not) and years in practice between classes. Findings from our Year 10 study suggest that primary care physician career typologies were stable over the decade as a whole, but we could not observe whether individual physicians transitioned to different career typologies during the decade.
In this project, we will leverage the unique panel nature of the North Carolina licensure data to conduct a latent transition analysis (LTA) of the 4,617 PCPs who were present in the data in both 2009 and 2019. LTA will allow us to examine if PCPs display career transitions between different typologies during the 10-year period and identify the factors associated with these transitions. Such an understanding could help policy makers identify if there are specific points in time, and physician characteristics, that are associated with an increased probability of transitioning from one career typology to another.
This project is/was supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under Cooperative Agreement for a Regional Center for Health Workforce Studies #U81HP26495. This information or content and conclusions are those of the author and should not be construed as the official position or policy of, nor should any endorsements be inferred by HRSA, HHS or the U.S. Government.
You must be logged in to post a comment.